Did you know that with Direct Access, you don’t need a doctor’s referral to go to physical therapy? Although Direct Access Laws vary a bit from state to state, you can see a physical therapist without a referral with most insurance groups. The hard part now is finding a physical therapist that meets both your treatment and pocketbook goals. If you have insurance, the first thought that probably comes to mind is looking through a list of physical therapy providers who are in your network. Although cost is an important consideration when looking for the right physical therapist, you first need to find the right physical therapy clinic for your recovery goals—then figure out the right payment options to fit with your needs.
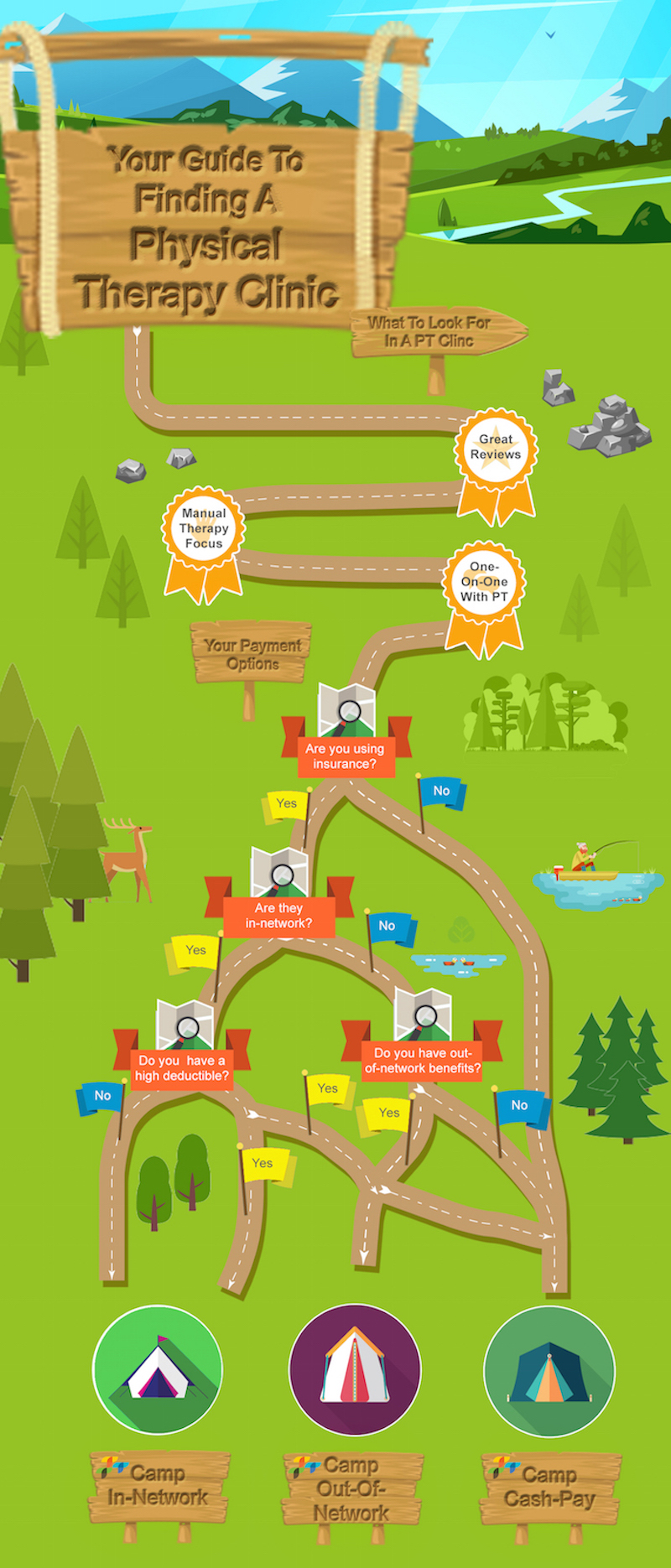
Start Mapping It Out: Finding Clinics That Fit Your Physical Therapy Needs
When researching various physical therapy clinics, look for quality clinics with good reviews. Find out how much physical therapy treatment time is spent one-on-one with the physical therapist who has a master’s (MSPT) or doctorate degree (DPT) vs. an aide or assistant. During your physical therapy treatment process, it’s key to receive manual therapy, a hands-on approach to physical therapy, from a licensed physical therapist and the proper education around your condition to avoid re-injury. If the majority of your physical therapy treatment is spent doing exercises with an aide, that is a red flag. Finally, look for clinics that offer post-physical therapy wellness and health services if you want the opportunity to continue beyond your treatment timeline.
In-Network: Going Down a Familiar Trail
When you find a physical therapy clinic that your insurance lists as being in-network, what that means is the clinic has a contract with your insurance company. The clinic has negotiated a lower price for the their services—the insurance company pays a specific fraction of the bill and you pay the rest (i.e. your copay). Going in-network for physical therapy may come with caveats in terms of what types of physical therapy treatment you can get. Some only approve physical therapy insurance for a certain amount of visits, ranging from 6 to 60 per year while others only approve coverage if you have an illness that’s led to a specific loss of function.
If you haven’t used any medical services this year, you will have to pay out-of-pocket for physical therapy and other medical services until your deductible has been met. If you’ve met your deductible for the year, that’s perfect. Overall, don’t feel obligated to go the in-network route if you can’t find an in-network physical therapy clinic that offers one-on-one treatments with a physical therapist—you do have other options.
Out-Of-Network: Unfamiliar Territory?
Most insurance companies have out-of-network benefits if you decide not to go with one of their in-network providers. If you’ve never used these benefits before, maneuvering through it may seem daunting, but it’s very similar to using your in-network benefits. Your clinic will bill insurance for your physical therapy treatment, same as in-network, and your insurance company will still pay a portion of the cost. Similar to in-network, they may only cover a certain amount per year. The only difference is that the clinic doesn’t have a specific contract with your health plan. Therefore, the price of the clinic’s services aren’t previously negotiated.
When compared to in-network, you may pay a slightly higher percentage of the total cost. But often, out-of-network benefits cover 60 to 80 percent of treatment costs. What’s compelling is that, depending on your physical therapy treatment, this may not be a whole lot different than if you had in-network benefits. You can ask a the physical therapy clinic you’re interested in to help you breakdown your specific physical therapy benefits so you can decide which treatment plan works best.
If you’re expecting physical therapy treatment that’s a bit more specialized or you simply want to make sure that you’ll have the opportunity to have highly effective, one-on-one treatments with a physical therapist, going out-of-network might be right for you if you can’t find an in-network provider that fits your needs. With out-of-network benefits, you may be paying a bit more out-of-pocket, but you’ll also get the quality of service you want and need. Depending on the treatment, going out-of-network may also result in less visits and time needed for recovery and an overall smaller expense.
Cash-Pay: No Detours Needed
For those who don’t have out-of-network benefits, insurance at all, or have high deductibles, paying directly is always an option. All the benefits of going out-of-network apply to paying directly. There are no third parties since you’re entering into a contract with the clinic itself. Most clinics may offer a bundled discount if you decide to go the cash-pay route, which may benefit those without physical therapy insurance, insurance in general, or high-deductibles.
With cash-pay, you’ll have no constraints when it comes to any methods or services that you need with your physical therapy treatment course; it all comes down to you. If you’ve heard about a high-quality physical therapy clinic, and aren’t covered for, you might decide to go the cash-pay route.
End Of The Journey
What is the main takeaway? To align your goals with your needs. It really comes down to your physical therapy treatment and which insurance or payment path works for you. Don’t be shy— feel free to ask your friends for any physical therapy clinic recommendations in your area. Google physical therapy clinics in your area to see who has the highest patient satisfaction. Don’t feel limited when it comes to finding the right physical therapy clinic for your treatment. Find the right path for your health goals.